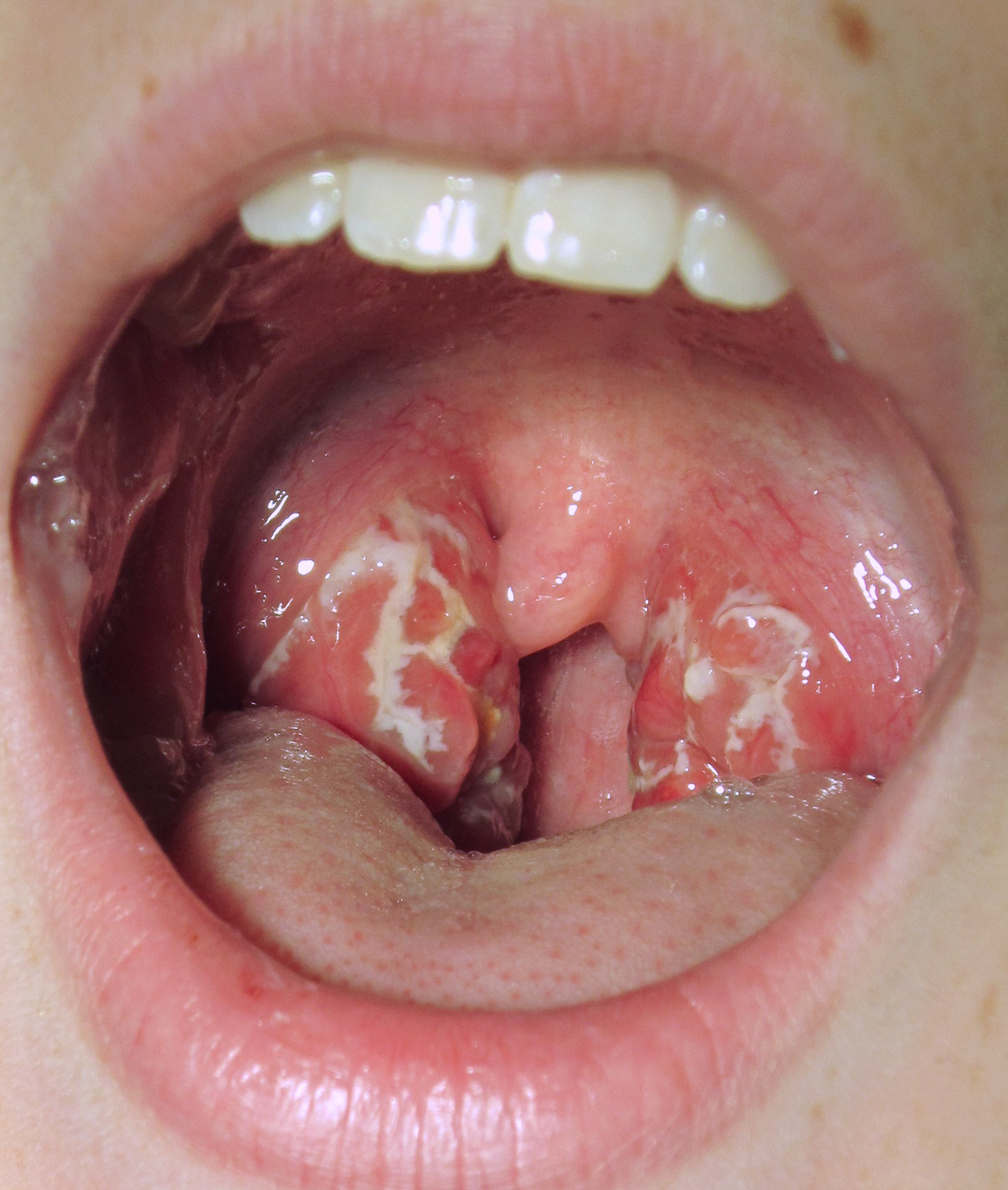
Some of the signs of strep throat will be visible. They may include:
-
white patches on the tonsils or throat,
-
dark red splotches or spots on the roof of the mouth, and
-
a skin rash.
Those white spots are pockets of pus. In addition, some patients may exhibit swollen, tender lymph nodes in the neck and some with fever above about 101-102 F. The signs and symptoms of strep throat are the same for both children and adults.
Although these signs may indicate strep throat, a visit to the doctor or a telemedicine consult is necessary to make a full determination. Strep throat cannot be diagnosed by visual signs alone. Click here to learn more about strep tests.
Adults are less likely to have strep throat than children. For children, their odds of a sore throat being strep throat are about 20% to 30%. For adults, the odds are more like 5% to 15%.
Streptococcal pharyngitis is strongly suggested by the presence of fever; tonsillar exudate; tender, enlarged, anterior cervical lymph nodes; and absence of cough (Centor criteria). Strep throat has an incubation period of 2-4 days and is characterized by sudden onset of sore throat, swelling of the glands in the neck, tiredness, fever, and headache. Younger patients may also develop nausea, vomiting, and abdominal pain. Acute sinusitis manifests as persistent runny nose and congestion, postnasal drip, headache, and fever.
The most important historical information to obtain in the evaluation of a sore throat is whether other symptoms of upper respiratory tract infection are present or not. Children with streptococcal pharyngitis do not have cough, rhinorrhea, or symptoms of viral upper respiratory tract infection. Indeed, the diagnosis of streptococcal pharyngitis can effectively be ruled out on the basis of the clinical findings of marked coryza (runny nose and congestion), hoarseness, cough, or conjunctivitis.
However, although these are important exclusionary criteria, the physician must be aware that signs and symptoms of strep may otherwise be nonspecific and that they vary widely depending on patient age, severity of the infection, and timing of the illness.
Relatively few localizing or constitutional symptoms may be present, such that the illness may be unrecognized (subclinical infection). Young infants do not present with classic pharyngitis. Streptococcal upper respiratory tract infections in infants and toddlers instead may be characterized by low-grade fever, anorexia, and a thick, purulent nasal discharge (so-called streptococcosis). Conversely, some patients may be toxic, with high fever, malaise (tiredness), headache, and severe pain upon swallowing.
Streptococcal toxic shock can be associated with pharyngitis; however, this is rare. Vomiting and abdominal pain may be prominent early symptoms simulating gastroenteritis or even acute appendicitis. Hence, streptococcal pharyngitis should be considered in a child with acute onset of abdominal pain. Because streptococcal pharyngitis is chiefly a disease of winter and spring and primarily affects children older than 3 years, fewer throat cultures should be completed in the summer and in children younger than 3 years.
Scarlet fever results from pyrogenic exotoxin released by GAS (Group A Strep) and is characterized by a scarlatiniform rash that blanches with pressure. The rash usually appears on the second day of illness and fades within a week, followed by extensive desquamation (skin peeling) that lasts for several weeks.
A history of recent exposure to another individual (e.g. classroom or household contact) with streptococcal infection is a helpful clue when looking at signs of strep.
Written By: Dr. Robert Rankins
Get our On-Demand Telemedicine Consult Package for Strep NOW and get diagnosed and a prescription filled within 24 hours without ever leaving your home! FREE Overnight shipping when you use the code “FREEOVERNIGHT” at checkout. Click HERE to start feeling better now!


